Everything you need to know about rosacea
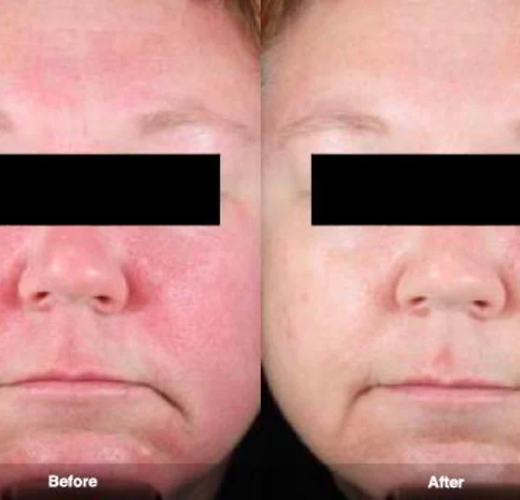
According to the National Rosacea Society, at least 16 million Americans struggle with this common skin condition, which is why it’s a hot topic among dermatologists and researchers alike. Beyond the tell-tale signs of facial flushing and blushing, recent studies have revealed more insights about the causes of rosacea—and the treatment options are rapidly expanding.
First and foremost, the American Academy of Dermatology updated their rosacea classification system in 2017. The previous system focused on four specific rosacea subtypes, although many patients experience the symptoms of more than one. Hence, the new classification system focuses on observable signs of rosacea:
- Erythematotelangiectatic rosacea: The most common form of rosacea that leads to a flushed appearance
- Papulopustular rosacea: Pimple-like lesions in the mid-face area
- Ocular rosacea: Redness, burning and itching of the eyes
- Phymatous rosacea: Skin thickening and other irregularities on the nose, chin, forehead, ears or eyelids
In addition to persistent redness on the cheeks, it’s important to consider flushing that occurs in response to specific triggers like sun exposure, stress, alcohol and certain foods. Pimple-like lesions are another symptom category as well. Yet another sign of rosacea is visible broken blood vessels, which often aren’t apparent to the naked eye in patients of color. Lastly, rosacea can have an effect on the eyes on the surrounding skin—and all of these symptoms need to be addressed to prevent them from progressing.
Until recently, dermatologists and researchers have been unable to pinpoint the root cause of rosacea. Hereditary and environmental factors have always been thought to be at play, and all cases of this skin condition involve inflammation, skin-barrier dysfunction, free-radical damage and vascular issues. New research is focusing on the role of the skin’s balance of “good” and “bad” bacteria, as well as impact of the gut microbiome and an increased presence of mites on the skin.
Although the specific cause (or causes) or rosacea have yet to be proven conclusively, treatment options have expanded significantly—and I approach every patient and case individually and try to find the ideal solution. The first step in keeping rosacea under control is avoiding your unique triggers, which are relatively easy to identify. If your skin flares up after having a glass of wine, eating spicy meal, exposure to heat or a stressful episode, you know what to avoid to help keep your rosacea in check. But oftentimes, trying to avoid these common triggers isn’t enough.
Any approach to rosacea treatment involves careful consideration of a patient’s unique triggers and symptoms. For mild cases of rosacea, over-the-counter barrier-strengthening ingredients such as niacinamide, feverfew, green tea, coffeeberry, aloe vera, soy, oatmeal and vitamin C have been shown to improve visible symptoms. Azelaic acid (which is also available in prescription strength) can help as well, and green color-correcting cosmetics also offer instant (although temporary) redness reduction.
In addition to light- and laser-based treatments, I have many medications to choose from depending on any given case. Topical minocycline is now available in a foam that integrates well into any skincare regimen. Other options include other prescription-based antibiotics and topicals like Elidel, MetroGel, Soolantra and Rhofade. More advanced cases of phymatous rosacea may require more aggressive surgical or ablative laser treatments.
Rosacea is a challenge for so many people, but you don’t have to sit back and concede defeat. Between managing your unique triggers and starting the proper treatment plan that can help keep your skin calm, cool and collected, it’s possible to keep rosacea under control—but it requires commitment and effort on your part.


